A Joint Approach to Breast Cancer Surgery: What It Means for You
6 min read

If you’re like the majority of women diagnosed with breast cancer, surgery is likely to be part of your treatment plan. Around half of women who need breast cancer surgery undergo a single or double mastectomy, while the other half have a lumpectomy. An increasing number of women are choosing breast reconstruction, a type of plastic surgery, after their mastectomy. Research shows that, when it is an option, getting reconstructive surgery at the same time as tumor removal surgery may have better outcomes for patients. Rocky Mountain Breast Specialists (RMBS) specializes in this joint approach to breast cancer surgery.
“It’s one big surgery instead of two or several surgeries,” said Dr. Gerlinde Tynan, FACS, board-certified breast surgeon specializing in surgical disease of the breast, mainly breast cancer, at Rocky Mountain Breast Specialists (RMBS). “You also have the benefit of having your team on the same page from the get-go.”
Breast Removal Surgery Basics
Mastectomy, or breast removal surgery, may be recommended by your surgeon for many different reasons, including the type of breast cancer you have and whether it has spread, your family or past history of cancer, or results of your genetic testing. There are several types of mastectomies, and your RMBS surgeon will work with you to ensure you know what your options are. The type of mastectomy you have may depend on the type of cancer you have, or it may be a personal choice you make with your surgeon. The basic types of surgery include:
- Simple (total) mastectomy: This surgery removes your entire breast, including the nipple. This surgery may include a sentinel lymph node biopsy, in which your surgeon takes a tissue sample from the sentinel lymph nodes under your arm nearest your tumor to check for cancer cells.
- Modified radical mastectomy: This surgery is like a simple mastectomy except it includes an axillary lymph node dissection, which is when your surgeon removes multiple lymph nodes and sometimes part of the chest wall.
- Nipple-sparing or skin-sparing mastectomy: While it is not possible for every person, RMBS prefers whenever possible (and desired) to use a nipple-sparing or skin-sparing mastectomy procedure. Nipple-sparing is a type of surgery in which the nipple, areola, and much of the breast skin is preserved while the inner breast tissue is removed. A skin-sparing mastectomy preserves as much skin as possible, but the nipple and areola are removed.
- Risk-reducing mastectomy (prophylactic mastectomy): During this surgery, a woman with no breast cancer or no cancer in her second breast chooses a mastectomy due to personal risk factors.
A bilateral mastectomy involves the removal of two breasts and can fall into any of the above categories. Surgery to remove lymph nodes may also be a part of any mastectomy except a risk-reducing one.
What to Consider About Breast Reconstruction
 Reconstruction surgery aims to create a “new” breast to replace the removed breast tissue and skin. There are several types of breast reconstruction surgery, but the most common type uses silicone implants, usually with a tissue expander. A plastic surgeon can also perform reconstruction with autologous tissue, which is skin and fat from elsewhere on your body such as your stomach or bottom. This type of surgery is also called a flap reconstruction.
Reconstruction surgery aims to create a “new” breast to replace the removed breast tissue and skin. There are several types of breast reconstruction surgery, but the most common type uses silicone implants, usually with a tissue expander. A plastic surgeon can also perform reconstruction with autologous tissue, which is skin and fat from elsewhere on your body such as your stomach or bottom. This type of surgery is also called a flap reconstruction.
“As surgeons, our top priority is cancer removal, of course,” Dr. Tynan said. “We want negative margins, we want to be able to tell patients, ‘All your cancer is gone.’ But our second objective is ensuring that patients are happy with their appearance after their surgery. My goal is to have a patient five years later look in the mirror and not feel disfigured but to feel good in their skin.”
Almost 138,000 people had breast reconstruction surgery in 2020, according to the American Society for Plastic Surgeons. Statistics show that breast reconstruction is more popular with women under 55, but plenty of older women also request the surgery.
Breast reconstruction performed at the same time a woman has a mastectomy is called an immediate reconstruction. If it happens later in the treatment process, it’s called delayed reconstruction. Some patients who need radiation after surgery may not be able to have immediate reconstruction.
If your breast cancer treatment requires surgery, your health insurance is also required to cover breast reconstruction.
An increasing number of women are choosing to “go flat” after a mastectomy rather than having their breast(s) reconstructed. In fact, a 2023 study showed that about 62% of women chose to go flat rather than have breast reconstruction. It’s a highly individual choice based on your personal preferences.
Why Immediate Reconstruction Makes Sense
Not everyone’s treatment plan is conducive to immediate reconstruction, but it’s a great option for many patients.
“There are still places in northern Colorado where patients do not have the option of having a plastic surgeon available at the time of their surgery and have to have their reconstruction later,” Dr. Tynan said. “But the cosmetic options are much more limited when you have delayed reconstruction than when you can have the two processes combined. You can spare more skin, and you can potentially keep the nipple areola complex.”
Only having one surgery is a definite benefit to immediate reconstruction, even when lymph nodes are removed. However, research indicates there are other benefits for most patients, such as improved quality of life after surgery.
“There is an overall psychological benefit to waking up after surgery with breasts,” Dr. Tynan said. “Yes, they may not look exactly like your old ones, but for many women, especially younger ones, the data has shown that it is beneficial compared to having a flat chest after surgery.”
A Joint Approach to Lumpectomies
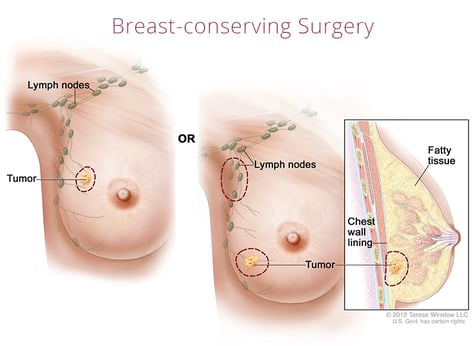 As conservative breast cancer management has increased, many women who would have had mastectomies 20 years ago now choose to receive lumpectomies instead. This type of partial breast removal surgery varies by patient, cancer type, and spread, but RMBS specializes in performing oncoplastic lumpectomy whenever possible.
As conservative breast cancer management has increased, many women who would have had mastectomies 20 years ago now choose to receive lumpectomies instead. This type of partial breast removal surgery varies by patient, cancer type, and spread, but RMBS specializes in performing oncoplastic lumpectomy whenever possible.
“For example, in partnership with the plastic surgeon, we might combine lumpectomy surgery with a breast reduction, and then do the other side to match,” Dr. Tynan said. “These types of oncoplastic lumpectomies can be complicated, and it is helpful for patients to be able to get reconstruction at the same time without having to go somewhere special.”
RMBS offers advanced oncoplastic lumpectomy techniques that preserve or enhance the appearance of the breast.
“We get to be a little bit artistic after we get the cancer out of there, trying to figure out how to reshape the breast,” Dr. Tynan said. “If we can, maybe we can make the breasts look even better than what we started with, so there’s that silver lining.”
The RMBS Difference
Choosing what kind of treatment for breast cancer to receive and whether to have surgery for breast reconstruction is an extremely personal decision. That’s why RMBS oncologic surgeons and plastic surgeons work hand in hand to make sure patients understand all their options.
“We work very closely together to make sure we’re all on the same page,” Dr. Tynan said. “Anytime you have good communication between providers, you have a better overall outcome.”
With immediate reconstruction, the two surgeons also work to limit pain and help speed recovery.
“A lot of patients come in thinking it’s going to be a very painful process, but one of the additional benefits of our joint approach is that we’ve developed a great pain management protocol,” Dr. Tynan said. “We have interventions that we do before surgery, and then during the procedure, I perform a nerve-block to decrease pain. Postoperatively we combine anti-inflammatories, a small amount of narcotics, and muscle relaxants to get patients through the first few days. A week later, most patients are only taking ibuprofen.”
If breast cancer surgery is in your future, consult the specialists at Rocky Mountain Breast Specialists to discuss your options. Find a breast specialist near you.