What are Colon Polyps and Are They Cancerous?
6 min read
Colon polyps are small clumps of cells that grow on the inside of your large intestine, or colon. While they’re fairly common in the large intestine, especially after age 45, most are harmless. Some can develop into colon or rectal cancer over time. Here we’ll look at the cause, types, and risk factors as well as how polyps are treated and what to do if one is found to be cancerous.
What Causes Colon Polyps?
In a healthy colon, cells grow in a routine way and die at the end of their useful life. Changes in your DNA can cause colon cells to divide when new cells are not needed. As the cells accumulate, they form into clumps and become polyps.
Most experts believe the risk of developing polyps is increased by both your environment and your family history. Since you can’t change your heredity, focusing on making good choices about your lifestyle can help prevent polyps. Smoking, obesity, alcohol, and eating a high-fat-low-fiber diet are all closely linked to polyp formation.
Related Reading: Ultra-processed Foods and Their Connection to Colorectal Cancer.
Are There Different Types of Polyps?
There are five main types of colon polyps that are classified after the tissue is examined under a microscope.
Types of polyps include:
- Adenomatous. This is the most common type that accounts for about 70% of all colon polyps. They can become cancerous over time.
- Villous adenoma. This type of polyp accounts for about 15% of all polyps. They are more likely to be cancerous. Because they’re typically flat, they’re also more difficult to remove.
- Sessile Serrated. Serrated polyps can become cancerous. The flat, larger-sized serrated polyps in the upper colon tend to be harder to detect. These polyps are usually precancerous.
- Hyperplastic. These polyps grow quickly and tend to stay small. They are usually not cancerous.
- Inflammatory. These are usually only found in people who have an inflammatory bowel disease (IBD). They’re not technically polyps because they are actually inflammation caused by IBD. They are unlikely to become cancerous.
Who’s At Risk for Colon Polyps?
While anyone can develop polyps, certain factors increase your risk, including:
- Age – being older than age 45; about half of all adults have polyps
- Inflammatory intestinal conditions such as ulcerative colitis or Crohn's disease
- Family history of colon cancer or polyps
- Genetic abnormalities (Lynch syndrome, familial adenomatous polyposis, serrated polyposis syndrome, and others) can cause polyps to form
- Smoking, especially when combined with alcohol
- Alcohol consumption: three or more drinks a day increases the risk
- Obesity
- Lack of exercise
- Eating an unhealthy, high-fat diet
- Race – colon cancer risk is higher in Blacks, compared to Whites
Learn more about whether colon cancer is hereditary.
Can Polyps Be Prevented?
Although it’s not known how to prevent colon polyps, the lifestyle choices you make can reduce your chances of developing them.
Making good lifestyle choices is also important in preventing polyps. Examples include:
- Eat a healthy diet that includes plenty of fruits, vegetables, whole grains, fiber, and a minimum of processed foods, red meat, and unhealthy fats.
- Limit alcohol or don’t drink at all
- Stop smoking and avoid second-hand smoke
- Maintain a healthy weight
- Exercise regularly, even as little as 20 minutes a day
- Ask your doctor if you need more calcium to help prevent the return of adenomas or Vitamin D to help protect against colorectal cancer
How Are Polyps Detected?
Most polyps are spotted during a colonoscopy. This test is part of the regular colorectal cancer screening process starting at age 45. If you have a family history or other risk factors for developing colorectal cancer, you should discuss screening at an earlier age with your doctor.
Related Read: When Should You Start Colon Cancer Screening?
The earlier polyps are found, the smaller they usually are. If cancer is found, an early diagnosis improves your chances for a cure and full recovery. Early detection of polyps is not difficult if you have regular screenings for colorectal cancer.
Which tests are used to find polyps?
There are several good procedures used to find polyps. The most common is a colonoscopy, but others may be used based on your personal history and health condition.
- A colonoscopy uses a flexible tube with a camera attached to check your colon for polyps. If any suspicious polyps are found, they can be removed during the procedure. Colonoscopies require that the bowel be clear before the procedure.
- Flexible sigmoidoscopy also uses a flexible tube to check the lower third of your colon for polyps. Polyps in the top two-thirds of your colon cannot be checked.
- Virtual colonoscopy uses a CT scan to check your colon from outside your body, although the bowel must be cleared like a colonoscopy. If abnormalities are found, you’ll also need a colonoscopy to remove them.
The doctor performing the colonoscopy, or other screening test, will typically remove polyps when they’re found so they can be tested for cancer cells. Your doctor will review the results with you to see if there are any additional steps you may need to take.
Can an at-home stool test detect a polyp?
At-home stool-based tests have become more popular, especially among those under 50. A stool sample is sent to the lab to check for blood in the stool. Newer stool tests also analyze your DNA to check for cancer. However, these tests cannot confirm whether blood in the stool is caused by a polyp. If blood is detected by the at-home test, a follow up colonoscopy is likely to be needed to find the source.
Does a Polyp Mean I Have Cancer?
Most polyps are harmless. However, the size of the polyp has shown to play a role in the likelihood of cancer developing. Most polyps are between 1 and 9 millimeters (mm) in size. Among those in a 2018 study published by the American Journal of Gastroenterology, only 3.4% were cancerous polyps. At 10mm or larger, the rate of cancer jumped to 13.4%.
This reinforces the importance of colonoscopies as part of colon cancer screening starting at age 45. By removing polyps that are a smaller size, there is a lower chance of cancer developing.
Can Polyps Cause Symptoms?
Most people with polyps don’t have symptoms, which is why it’s so important to have regular screenings to check for them. However, larger polyps may sometimes cause these symptoms:
- Blood or mucus in your stool
- Changes in your normal bowel habits, such as constipation or diarrhea lasting longer than a week
- Bleeding from the rectum
- Changes in stool color, such as red streaks or black stools
- Anemia, caused by chronic bleeding from polyps, which can introduce fatigue and shortness of breath
- Pain or stomach cramps, caused by large polyps, that partially block your bowel
- Unexplained weight loss
How Are Colon Polyps Treated?
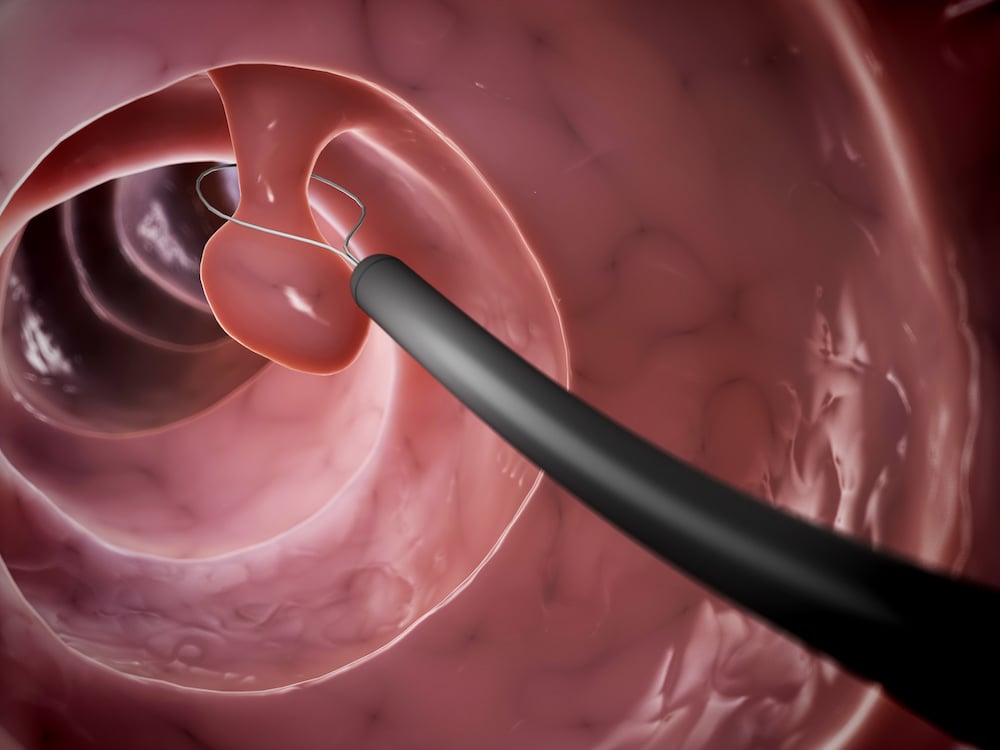
In most cases, the polyps are removed painlessly during the colonoscopy. This is called a polypectomy. The most common removal methods include using a wire loop to cut off the polyp or using an electrocautery device that burns through the base of the polyp.
Surgery may be needed if polyps are too large or pose too great a risk to be removed during a colonoscopy. Minimally invasive surgery to remove the cancer can be done with a laparoscope through a small incision in the abdomen.
After polyp removal, you may need to have follow-up care depending on the type of polyp you have:
- Small hyperplastic polyps in your lower colon usually don’t need follow-up until you have another colonoscopy in 10 years.
- Hyperplastic polyps in the upper colon usually require more frequent repeat colonoscopies.
- Adenomatous polyps need a repeat colonoscopy; timing is based on the polyp’s size, number of polyps, and their appearance.
- If you have a personal or family history of polyps, you have a greater risk of developing new polyps. Patients who’ve had an adenoma have a 30% to 40% risk of recurrence within three years.
Your doctor will discuss the timing of future screening based on these factors.
What if the Biopsy Shows the Polyp is Cancerous?
If a polyp is biopsied and is found to be cancerous, you will need to see an oncologist. The good news is that colorectal cancer that was found early during a screening colonoscopy usually means it’s a very early stage and highly treatable. In fact the five-year survival rate is 90% for patients with localized colon cancer.
At Rocky Mountain Cancer Centers, we have specialists in colon and rectal cancers who are available for a consultation. Find a location in Denver, Boulder, Colorado Springs, or throughout the Front Range to schedule an appointment.

