Breast Cancer

-
Explore Breast Cancer
- Overview
The Latest Treatments & Experienced Breast Cancer Doctors
Every breast cancer diagnosis is unique – just like you. That’s why Rocky Mountain Breast Specialists focuses on providing state-of-the-art treatment and expertise while personalizing care to fit your needs. Our entire team of experts are dedicated to your personal health and wellness goals. Find the right breast cancer specialist in Colorado to care for you.

Every one of us with you, every step of the way.
From your very first appointment through each step of your treatment plan, Rocky Mountain Breast Specialists is by your side. We understand that a breast cancer diagnosis can be confusing and scary. With Rocky Mountain Cancer Centers, you can be confident that you will be supported by a compassionate and experienced team of breast cancer experts and receive the most advanced treatments available. One of our favorite roles? Supporting your ongoing care as a breast cancer survivor.
Diagnosing Breast Cancer: What's Next After a Mammogram?
What to Expect After a Breast Cancer Diagnosis
If you’ve been diagnosed with breast cancer, you likely have many questions about the coming days, weeks, and months. We are here to help answer these questions and address your concerns, so you feel empowered and prepared for your first appointment.
2,400+
New Breast Cancer Patients Treated Each Year at Rocky Mountain Breast Specialists
Understanding Breast Cancer
Selecting Your Breast Cancer Specialists

Who is a Part of Your Breast Cancer Care Team?

Choosing Your Breast Cancer Surgeon

Experiencing a Team Approach to Breast Cancer
Personalized Breast Cancer Treatments at RMBS
Breast Cancer Frequently Asked Questions
In general, the sooner you can start treatment the better. However, in most cases you have time to review options and meet with two different oncology teams to compare their plans and determine which is a better fit for you. Most patients also need some additional tests run before treatment begins. This helps determine the extent of the breast cancer in the body and makes it possible to decide which treatments will likely be effective. If you received a breast cancer diagnosis, feel free to schedule a consultation with one of our breast cancer doctors at an RMBS in the Denver, Colorado Springs or Boulder areas. Our experienced team will walk you through their best recommendation and explain the timing of treatments.
Yes, most people have a choice on where to receive breast cancer treatment and who will perform the surgery. You may have been diagnosed through a mammogram performed at a hospital system. That facility will likely recommend you see one of their breast cancer surgeons or oncologists next. You can evaluate your options outside of the referral. You might also consider the following:
- Total cost for treatment - Even with insurance treatment can be costly. Choosing an independent cancer center like RMCC is proven to lower the total cost of treatment compared to a hospital outpatient department.
- Appointment availability - If you are looking at several weeks for a first appointment we recommend you evaluate your options. Our highly rated breast cancer doctors and surgeons work hard to make appointments available for new patients – including second opinions.
- Location of the cancer center - During treatment you are going to visit the cancer center often for appointments, treatments and follow ups. It's helpful to receive your care close to home. RMBS provides coordinated care through our network of 19 locations in Colorado.
If breast cancer runs in your family, your chances of getting it are higher. Most women with a family history don’t have an inherited mutation in the BRCA1 or BRCA2 gene. In fact, BRCA mutations are related to only 5-10% of all breast cancer diagnoses. But if several family members have had breast cancer or other cancers like ovarian, pancreatic, or prostate cancer, there could be a family-related genetic change. Our high-risk breast clinic can help you develop a screening plan that's right for you based on your personal risk factors.
The RMBS oncologists may recommend treatment before breast cancer surgery. This is called neoadjuvant therapy. The decision to give treatments before surgery depends on the type and stage of breast cancer. Patients with triple-negative or HER2-positive breast cancer often receive treatments like chemotherapy, hormone therapy, or targeted therapy first. If the tumor is large, neoadjuvant therapy can shrink it so that only breast-conserving surgery is needed rather than a mastectomy. The best order for treatments will be evaluated by our team and discussed with you before therapy begins. Feel free to ask questions about the goal of each treatment and the timing of each.
Depending on the stage and type of breast cancer, your oncologist will develop a treatment plan. If you will have surgery and only receive radiation therapy afterwards, there's a high likelihood you will keep your hair. For patients whose cancer is large or has progressed to the lymph nodes, one or more systemic treatments may be recommended such as chemotherapy, immunotherapy, or targeted therapy. The chemotherapy often used to treat breast cancer is known to cause hair loss. This is something you can plan for and possibly prevent using cold-capping technology. Learn more in our blog: Understanding Hair Loss from Breast Cancer Treatment.
Talk to your breast cancer doctor about your specific treatments and hair loss as well as other side effects you might expect.
Our financial counselors will review your insurance plan's cancer benefits and then meet with you to discuss what will be covered and any out-of-pocket expenses. It's important to note that receiving cancer care at an independent cancer center like Rocky Mountain Breast Specialists results in a lower cost for patients when compared to cancer care at hospital outpatient departments. According to the Community Oncology Alliance, cancer treatment can cost up to 50% less in an independent oncology practice compared to a hospital-affiliated outpatient department.
Receiving affordable cancer care does not mean compromising on quality. We provide the same quality of care as hospital-affiliated oncology departments using advanced technologies and personalized treatments at a more affordable price.
Clinical trials offer access to new treatments for breast cancer that aren't widely available yet. RMBS participates in several breast cancer clinical trials, providing patients with opportunities to explore innovative treatments. Not every patient qualifies, but we are happy to review options for you and make a recommendation for participation if you qualify for one or more trials. Talk with your oncologist about whether a trial may be right for you.
For over 30 years, RMBS has been a leader in delivering world-class cancer care to patients across Colorado. Our oncologists, breast surgeons, and advanced practice providers were trained in the most renowned cancer centers in the United States and beyond, bringing their expertise to you. They are dedicated to being innovative and forward-thinking, never settling and always seeking the right treatment for their breast cancer patients. Meet our breast cancer specialists.
Recurrence is a valid concern for breast cancer patients. The type of breast cancer and the stage at diagnosis impact the likelihood of breast cancer recurring.
If you were diagnosed with hormone-positive breast cancer, your oncologist may suggest you use hormone therapy for five years or longer after your treatment is complete. These drugs are proven to reduce the likelihood of recurrence if used as prescribed. They can cause some side effects, however. Be sure you discuss those with your cancer care team rather than simply discontinuing use if you want to reduce your breast cancer recurrence risk. Read our blog: The Pros and Cons of Hormone Therapy for Breast Cancer.
There are other ways you can contribute to your overall health that lower breast cancer recurrence risk:
- Eat a balanced, anti-inflammatory diet: Focus on foods with no preservatives, lean proteins, low or no sugar, and plenty of water.
- Stay physically active: Obesity is linked to hormone-positive breast cancer recurrence. By incorporating exercise into your routine, you can lower your weight and reduce fatigue during and after treatment.
- Lower your alcohol intake. Even small amounts of alcohol can increase levels of estrogen and other hormones associated with breast cancer.
- Quit smoking: If you're a smoker, it's time to quit to not only lower your risk of cancer recurrence, but to lower your risk of several other conditions including heart disease.
- Manage stress: Consider mindfulness, counseling, or support groups.
Be sure you go to all of your follow up appointments after treatment is complete. The cancer care team will run tests to look for signs of recurrence.
Breast Cancer Education Center
Helpful Information About Breast Cancer from Our Blog

Hormone Replacement Therapy & Breast Cancer Risk: What Women Should Know
If you’re in your mid-forties or older, it’s likely you’re experiencing symptoms of perimenopause or menopause. Many women experience fatigue,...

Living with Stage IV Breast Cancer
Metastatic breast cancer - also known as Stage IV breast cancer - is complex to treat and can be difficult to navigate after diagnosis. While not...

Pros and Cons of Hormone Therapy for Breast Cancer
Breast cancer is a broad category that encompasses several different types of the disease. One specific type is hormone receptor-positive (HR+)...

How the Type of Breast Cancer Affects the Treatment You Receive
A breast cancer diagnosis is actually more complex than it may seem. There are many different subtypes of breast cancer. The specific subtypes...
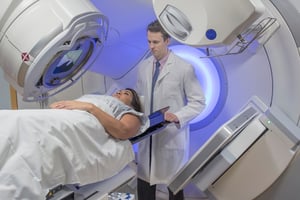
Hypofractionated Radiation for Breast Cancer
Radiation therapy is commonly used to treat breast cancer, usually in conjunction with other forms of treatment, known as a concurrent treatment....

Does Race Affect Your Breast Cancer Risk?
Breast cancer is the most common type of cancer among women and impacts all ages, races, and ethnic backgrounds. However, data shows that while white...

“Going Flat” After Mastectomy: Is It Right for You?
Choosing to have a mastectomy is a big decision. Once you have taken this step, you and your breast cancer surgeon will discuss the options for...
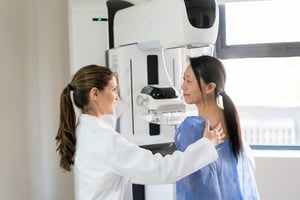
What You Should Know About the Types of Breast Cancer Screening
Most women don’t experience signs or symptoms of a tumor developing in their breasts. Fortunately, breast cancer screening is widely available,...

Cancer and Breast Implants: Is There a Connection?
Do breast implants cause cancer? Can you get a mammogram if you have breast implants? What happens if you receive a breast cancer diagnosis and you...
Find a Location
Learn More About Breast Cancer
Is Your Breast Cancer Hereditary?
Whether you or a loved one has been diagnosed with breast cancer, it can be important to know if the cancer has a genetic connection. While only 5-10% of all breast cancer cases are hereditary, a genetic counselor can assess your risk and help you take next steps.
Find OutSigns & Symptoms of Breast Cancer
Detecting breast cancer in its earliest stages is best, when treatment is more likely to offer better outcomes. Learn the signs and symptoms of the disease for better detection.
Read MoreRMBS Breast Cancer Survivor Stories of Inspiration

HER2-positive Breast Cancer Patient Paves the Way for Future Treatment
Nancy Chapin tackles cancer the way she approaches everything in life—head-on and with a healthy dose of humor. At age 81, Nancy has undergone...

A Hero Among Us: Cancer Survivor on a Mission to Help Others
Someone who battles cancer is a special type of person. In fact, some might even call them a superhero. They have the ability to overcome obstacles...

Adventuring on with Metastatic Breast Cancer
Pinder Gill has more hiking trails to complete, more countries to explore, and more memories to make with her family. In short, the 46-year-old tech...

Breast Cancer Survivor Says Get Your Mammogram
In 2017, Lakewood, Colorado resident Lois Brady wasn’t feeling very well, so she scheduled an appointment with her primary care provider. What she...

Cultivating Something New: Life After a Breast Cancer Clinical Trial
Tracy Calocci wasn’t born in Colorado, but after living in the state for more than 25 years, she can’t imagine calling any other place home. She...

Actively Opposed: One Woman’s Stand Against Metastatic Breast Cancer
Staying active has always been a way of life for 66-year-old Denver resident Alice Moring.*
“I grew up playing football, baseball, and basketball,”...

Triple-Negative Breast Cancer: Treated Just in Time
Days before her 40th birthday, Rebekah Layton, a mother and pastor from Highlands Ranch, was chatting with her husband and some friends. During the...

Free of Breast Cancer for 17 Years Thanks to the Team at RMCC
In April 2005, Colorado Springs resident Christy Sawina noticed a lump while performing a breast self-exam. Her last mammogram was years earlier, so...

Kathryn Gray Is Back on Track After Breast Cancer
For Kathryn Gray, running is a way of life. The Castle Rock, Colorado, resident ran her first road race around age six. Since then, she has trained...
